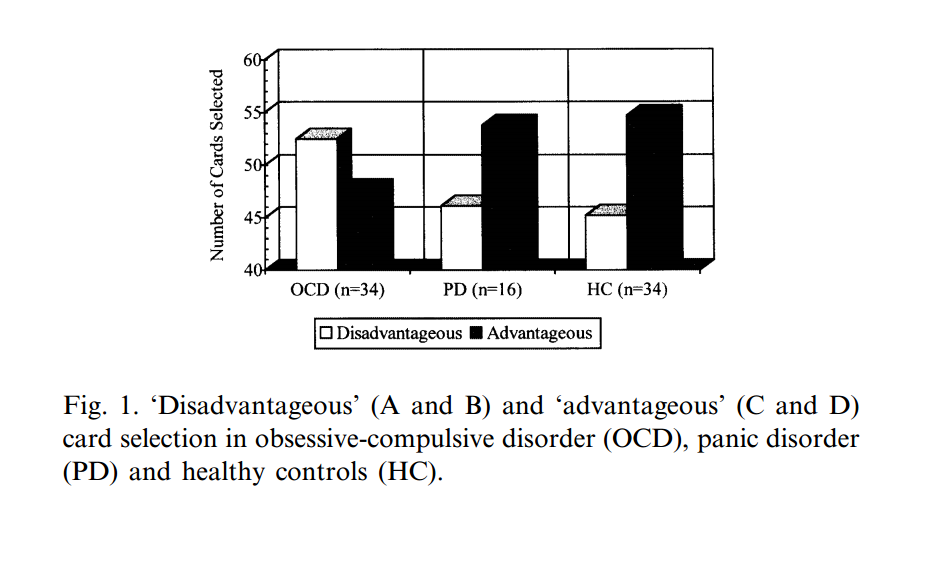
When people think about OCD they may think about excessive germaphobia, hording, or checking. Rarely is OCD conceptualized in terms of a dysfunction in decision making. But that may be just what it is. A person with hoarding symptoms cannot decide whether throwing away a shoelace or an old […]
